
Continence, urology and colorectal (CUCS)
We support adults with bladder, bowel or stoma and catheter problems.

About the continence, urology and colorectal service
We provide assessment and treatment of adults with bladder, bowel or stoma and catheter problems. We support patients and their family or carer to self-care and control their symptoms.
We hold specialist clinics across the city and see patients at home if necessary.
Who’s it for?
The continence, urology and colorectal service provide evidence based high quality continence care to adults (age 16 or over unless under care of children’s services when care will be transferred at age 19 years).
A nurse with specialist training in bladder and bowel care will talk to you so you can both decide the best way we can help. Bladder and bowel problems are very common and there is no need to be embarrassed. Simple tests may be necessary to find out what is causing your problem and so we can agree the best possible treatment. We will discuss this with you. We may need to carry out a physical examination. We will discuss this with you at your appointment and only perform an investigation you are happy with.
The service also provides advice and education to neighbourhood teams and other health, social or informal carer.
Examples of our care include:
- Accessible care for people with bladder, bowel, pelvic floor and stoma problems
- Specialist nursing care for patients with complex bladder, bowel, stoma and catheter problems
- Providing advice on other containment products
- Prescribing appropriate, cost-effective treatments
These are only available after completion of suggested treatment program.
Referrals
Most referrals come to the continence, urology and colorectal service by a GP, Neighbourhood team or hospital, although patients may refer themselves to the service using a self-referral form. GPs or other healthcare professionals refer patients by sending a completed referral form to the service.
Attending your appointment
Useful information
The aim of the service is to improve the symptoms of any bladder or bowel dysfunction, giving the person back an element of control, and reducing any impact it may be having on their, and their carer’s, quality of life.
Bladder and bowel problems in adults are common, affecting males and females of all ages. Common problems may include urgently needing to pass urine, incontinence, or difficulties fully emptying the bladder or bowel. The aim of this booklet is to provide you with some simple information to help you improve your bladder or bowel symptoms while you wait to be seen by a member of our team.
Here is some advice which may help reduce your symptoms.
Bladder
If you experience bladder pain or pass any blood when passing urine, it is important that you inform your GP and do not wait to be seen by our service.
Most of us urinate between 4 to 8 times per day. Getting up once a night if you are under the age of 50 and twice per night over the age of 50 is considered ‘normal’ bladder behaviour.
Needing to go more than eight times a day or waking up in the night to go to the bathroom could mean you are drinking too much and (or) too close to bedtime. If you are getting up more than 1 to 2 times a night, try and have your last drink 1 to 2 hours before you go to bed.
Try sitting with your feet up when you are at home, have a rest with your feet up or on the bed for at least an hour in the afternoon.
Make sure you drink enough fluids: 5 to 8 mugs (3 to 4 pints, 1.5 to 2 litres per day). Avoid fluids which irritate the bladder such as caffeine (including tea, coffee and hot chocolate), fizzy drinks (including fizzy water and juices), citrus juices and alcohol.
The best types of fluid to drink are still water, decaffeinated fluids, still dilute juices (not fizzy). Hot chocolate and green tea will make you urinate more, so try Ovaltine or Horlicks as a replacement.
Did you know? The less you drink, the more you urinate. This is because concentrated urine irritates receptors in the bladder which make us want to get rid of urine faster.
If you or your relative struggle to drink recommended amounts, you could consider soup, jelly or milk puddings or you could consider buying Jelly Drops, they look like sweets but are 95% water.
- Email: hello@jellydrops.com
- Visit the Jelly Drops website
If you are urinating frequently, try to increase the amount of time between each visit to the toilet by using pelvic floor contractions (see exercises below) and hold on a little longer to increase how much your bladder can hold. Start with 5 to 10 minutes at a time and then slowly increase it.
If you have an urgent desire to get to the toilet and sometimes leak from your bladder before you get there, try and use your pelvic floor to reduce the sensation. When the urge comes on, sit or stand still and use your pelvic floor muscle to try and settle the urgency before going to the toilet. It does take practice but is very effective.
If you find that you leak on coughing, sneezing, standing, lifting or walking, this could be because of a weakened pelvic floor muscle. Strengthening your pelvic floor muscle can help with this.
Your pelvic floor muscles surround the bladder and urethra (the tube that carries urine from your bladder out of your body) and control the flow of urine as you wee.
Weak or damaged pelvic floor muscles can cause urinary incontinence, so exercising these muscles is often recommended.
How to find your pelvic floor muscle
- Sit on a chair.
- Squeeze your bottom muscle (anus) as if you are trying to stop wind from passing. Try not to use the muscles in your buttocks or thighs.
- For women: Draw that squeeze forward to tighten the vagina.
For men: Draw up the squeeze and see or feel your scrotum lift (men sometimes find it easier to stand in front of a mirror to see this lift). - Hold this squeeze (this may only be for 2 to 5 seconds).
Repeat 3 to 5 times. - After this, complete ‘fast squeezes’, this is when you squeeze up and immediately relax. Repeat 3 to 5 times.
- Try and develop a routine to ensure you do these exercises three times per day, gradually increasing the length of the hold until you can lift and hold for 10. Repeat this 10 times.
Bowels
If you have:
- noticed any blood or mucus in your poo.
- have unexplained weight loss.
- changes in your poo, such as having softer poo, diarrhoea or constipation that is not usual for you for longer than four weeks.
Please bring this to the attention of your GP and do not wait to be seen by our service.
If you are experiencing problems with your bowels, you may find the following suggestions helpful
Ensure you drink plenty of fluids
Follow the fluid guidance above.
Eat regularly
Ensure you have 3 meals a day. Skipping meals in case you have an accident does not work and confuses your bowels. Eat a balanced diet which includes fruit, vegetables and fibre. Aim for 5 a day.
Porridge or Weetabix are good bulkers for your poo and can help to keep stools soft and formed.
Try to establish a good routine
As a service we recommend trying the ‘morning routine’. Wake up and have something to eat and drink. Once you have done this get dressed and (or) exercise, then try to open your bowels.
Toilet position
If safe to do so, place feet on a stool or a ’squatty potty’ so that your knees are higher than your hips.
If you do not have a squatty potty, you could also use an upside-down wash bowl or other product that is at a safe height for you.
Medication
Medication can affect both bladder and bowels, for example, stop you from urinating, increase frequency and (or) cause loose stool or constipation. If you have any concerns about medication, contact your GP.
When did you last have a medication review?
If you have not, please arrange one as this may improve your symptoms.
Do you buy any medications over the counter?
Any medications bought over the counter can interact negatively with prescribed medication.
Please check with your pharmacist.
Further support and advice for incontinence
Some people need to access toilets when out and about more quickly.
Have you thought about applying for a blue badge?
If you have mobility problems, this may help reduce time taken to reach a toilet safely.
Have you thought about a RADAR key for accessible toilets?
These are available to anyone registered with a disability and can be sourced for free through your local authority. Contact RADAR on:
- Email: sales@Radarkey.org
- Phone: 01395 222 588
They are also available online and from Motability shops. This may incur a small charge.
Clinical waste
If your disposal of incontinence products is equal to a household with two babies nappy use, you can dispose of your containment in your general waste bin. Some patient’s clinical waste is greater. If so, you can contact the Council’s waste disposal service on phone: 0113 222 4406 to arrange a second black bin if needed due to continence, this is a free service.
Allowances
If you are in receipt of your pension (plus or minus any private pension) and have incontinence and mobility issues, you could be entitled to ‘Attendance Allowance’ which is the only non-means tested allowance available.
For more information, please contact 0800 7310 122. They may send you a form which you will need to complete.
Water rates company
If you have more washing due to your incontinence, or increased hygiene needs, please contact your water company for a form to complete which may reduce your payments to them.
Are you a vulnerable person?
If so, this can be registered with your gas and electric company.
Containment products (incontinence pads)
Continence, urology and colorectal service (CUCS)
We much prefer to treat symptoms before we consider containment products. You will receive an in-depth assessment during your first appointment to assess your current needs. However, there are times where containment is the only help that we can give.
It may help to purchase containment prior to your appointment. Pads can be bought for different levels of incontinence.
If you suffer from light incontinence, products such as washable incontinence underwear can be purchased to prevent furniture and clothing from becoming soiled. Other products such as Kylie sheets can also be purchased (online) to protect furniture.
Incontinence pads can be purchased from various sources including supermarkets, charity shops and online (Amazon).
For gentlemen: There are other body worn products which may help prevent the need for incontinence pads. These can also be supplied on prescription. If you would like further information on this, there is a self-referral route from the Nightingale website or phone: 0800 304 7434.
Nightingale can arrange a visit or telephone call with a company nurse who can provide you with more information and complete an assessment with you for a sheath or body worn systems.
Further information on how to fit the incontinence pads
Tena comfort normal, plus, extra and super
These should be folded in half lengthways. However, these incontinence pads are held in place by firm fitted underwear.
Net fixation underwear can be self-purchased if these are the preferred option to underwear.
Click here for a video guide on how to fit TENA comfort on a user lying down.
Tena slip range
These pads are secured with sticky tabs at the sides and come in various absorbencies and sizes. They are usually more suited for a person who can no longer use the toilet independently or is cared for or nursed in bed.
Watch the video guide on how to fit TENA slip on a user lying down.
Watch the video guide on how to fit TENA slip on a user standing up.
Washable incontinence products

We recommend having 3 of these washable bed pads for use in rotation whilst one is in the wash, you can have one on the bed, as well as a spare.
Kylie and Kanga
You order from Kylie and Kanga:
- Phone: 0115 978 6111Please order by calling the number provided
- Opening hours: Monday to Friday from 8am to 5:30pm
Note: We are not open on weekends.
Useful addresses and contacts
Age UK advice line
- Phone: 0800 6781 602
Age UK continence shop
They sell disposable and washable products and all profits are used within the charity.
- Age UK Continence
- Phone: 0800 0461 501
Bladder and Bowel UK
- Phone: 0161 214 4591
- Email: bbuk@disabledliving.co.uk
Capatex Care
They sell disposable and washable products including the Kylie and Kanga range.
- Phone: 0115 978 6111
- Capatex website
Menopause Matters
This is a website offering detailed information on menopause which is research based, helping to sort fact and myth.
Motor Neurone Disease Association
- Phone: 01604 250 505
- Email: enquires@mndassociation.org
MS Trust
- Phone: 0800 032 3839
- Email: ask@mstrust.org.uk
- MS Trust website
MS Society
- Phone: 0808 800 8000
- Email: helpline@mssociety.org.uk
Parkinsons UK
- Phone: 0808 800 0303
- Email: hello@parkinsons.org.uk
Spinal Injuries Association
Stroke Association
- Phone: 0303 3033 100
- Email: helpline@stroke.org.uk
Support my life with Care and Repair
Based in Leeds. They sell continence products, but also can arrange for adaptions to your home such as grab rails and a keysafe.
Telecare
For either a pendent and wrist alarm system should you fall, call for assistance.
- Phone: 0113 3782 991
- Email: telecarereferrals@leed.gov.uk
Tena Direct
They sell the Tena range which we prescribe in Leeds if an assessment results in containment or pads being required.
- Phone: 0800 393 431
- www.tenadirect.co.uk
William Merritt
This is a specialist centre that can help with the purchase of furniture and equipment such as raiser or recliner chair, mobility aids, kitchen aids. They will ask companies to send samples of equipment you can go and try at their centre.
- Phone: 0113 350 8989
- Email: info@wmdlc.org
- William Merritt website
The continence, urology and colorectal service (CUCS) provides high quality care to patients.
If you think you may be eligible for a home visit please read this leaflet before applying.
Benefits of attending a clinic appointment
- The clinic offers specialist treatment and has diagnostic equipment that is not available for home visits.
- You will be examined or treated on a specially designed couch to ensure you are comfortable during treatment.
- You are able to arrange your clinic appointments to suit your needs.
- You will be seen quicker.
- Patients who really need a home visit will not have to wait as long.
Providing care for housebound patients is an important part of our service.
Recent research shows that healthcare professionals are at risk of developing musculoskeletal disorders, such as back, shoulder, neck, wrist, hand, hip and knee problems.
These risks are much greater for staff when providing care in a patient’s home.
To provide patients with safe and effective care and minimise the risk of injury to our staff, we need to ensure they work in a suitable environment.
Patients eligible for a home visit
The following criteria for a home visit are based on the Department of Health ‘Eligibility criteria for patient transport services’.
Following consultation this criteria has been adopted by the continence, urology and colorectal service.
You may be considered for a home visit if the following apply:
- It would be detrimental to your condition or recovery if you were to travel to the clinic.
- Your medical condition affects your mobility so you are unable to travel without using an ambulance, for example, unable to take a car or taxi.
Patients not eligible for a home visit
You will not be eligible for a home visit if you are able to go out either by taxi, private car, motorised scooter, bus or use the Access Bus to visit any of the following:
- GP
- Shops
- Relatives
- Pick up your pension
- Hairdresser or barber
- Dentist or optician
- Phlebotomist or nurse, or
- Luncheon club.
In these circumstances, you will be asked to attend your clinic appointment for your continence care.
Getting to the clinic
- Use public transport. Metro: 0113 245 7676 or visit the Metro website.
- Use or share a taxi. See Yellow Pages or Thompson Local.
- Family and friends are often willing to help out.
- Combine a clinic appointment with another trip such as shopping, personal or health appointments like going to the doctor or hairdresser.
- If you use the Access Bus to go shopping arrange your continence appointment for the same day. Contact Access Bus on 0113 348 1903.
- Contact a local voluntary agency that may operate a voluntary driver scheme.
Please refer to ‘The A-Z health and social care information in Leeds: Mini guide for older people and disabled people’ available in local libraries or Leeds City Council social services. - Leeds Alternative Travel will take you door to door for a small charge. Call on 0113 386 8880
- If you receive the high rate mobility component of the Disability Living Allowance or War Pensioners Mobility Supplement you must use this to pay for your transport costs to clinic.
Change in circumstances
If your situation changes and you are able or unable to attend a clinic appointment, please contact the continence, urology and colorectal service.
The nurse will review your eligibility for a home visit at each appointment.
If you are no longer eligible for a home visit, we will arrange for you to be seen at a clinic appointment.
How to apply for a home visit
To apply for a home visit you will need to complete a mobility questionnaire that should be returned to the address on the form.
The continence, urology and colorectal service (CUCS) is for anyone 16 years or older who experiences a bladder, bowel or stoma problem.
A nurse with specialist training in bladder and bowel care will talk to you so you can both decide the best way we can help.
Bladder and bowel problems are very common and there is no need to be embarrassed.
Continence products may be provided by the health service after an assessment and completion of suggested treatment programmes.
Continence products can be purchased from local shops, supermarkets, chemists, online or over the telephone and then delivered to your home from several companies or charities.
Company or charity details
Age UK
- Phone: 0800 046 1501
- Opening hours: Monday to Thursday from 8am to 6pm, Friday from 8am to 5:30pm, Saturday from 9am to 1pm
- Age UK Continence website
Support My Life (Managed by Care and Repair)
- Phone: 0113 240 6009
- Opening hours: Monday to Friday from 9am to 4pm
- Care and Repair website (you can also visit their shop at 323 Roundhay Road, Leeds, LS8 4HT)
Kylie and Kanga
- Phone: 0115 978 6111
- Opening hours: Monday to Thursday from 8:30am to 5:30pm, Friday from 8:30am to 5pm
- Kylie and Kanga website
Tena Direct
- Phone: 0800 393 431
- Opening hours: Monday to Friday from 8:30am to 5pm
- Tena Direct website
Maintaining a healthy bowel is one of the essentials of healthy living, so it is important to know what can cause unhealthy and poor bowel habits. Poor bowel habits can lead to constipation, and (or) faecal incontinence which is often uncomfortable and can be painful. The following information looks at several key factors, which help maintain a healthy bowel.
Normal bowel function
The bowel is part of the digestive system and its role is to digest the food that we eat, absorb the goodness and nutrients from the digested food into the blood stream, and then to process and expel the waste products from the food that the body cannot use. As long as stools are passed without excessive frequency, with minimal effort and no straining, and without the use of laxatives, bowel function may be regarded as normal.
How often should the bowel be emptied?
There is no right or wrong answer to this. There is a very wide range of ‘normal’ bowel function between different people. Only a minority of the population has a bowel action once per day. Some people go several times a day and others have several days between bowel actions.
Reviewing medication
Be aware, some medications can have an effect on how your bowels work. If in doubt, organise a review of your medications with your GP or pharmacist. Medication such as pain killers, antidepressants and iron tablets can cause constipation. Medications such as diabetic tablets, antibiotics or antiacids can cause loose stools (poo) which can lead to faecal incontinence. Discuss your laxative use with your healthcare professional and always let them know about medicines you buy from a chemist or on the internet. More than one laxative may be used to relieve your constipation. Too much laxative can make your stools loose. Your clinical nurse specialist will complete an assessment and support you with treatment and (or) bowel management to reduce the risks of constipation, poor emptying and (or) faecal incontinence to enhance your quality of life.
What may go wrong?
A number of things can go wrong with your bowels that may cause constipation or faecal incontinence. The nurse specialist will discuss with you what is wrong in your case.
What will help to make your bowel healthier?
- Diet
- Exercise
- Morning routine
- Toilet position
- Defaecation techniques
- Medication review
Dietary fibre
Fibre is the non-digestible part of plant foods which passes through the stomach and bowel providing bulk. Fibre is important for maintaining a healthy bowel and can improve stool consistency and regularity. Most of us do not eat enough fibre in our diets. You can improve your fibre intake by including more of these foods:
Bread and cereals
- Start the day with a high fibre cereal (for example, Weetbix, wholewheat cereals, porridge, muesli) or wholemeal or wholegrain bread.
- Stock up your cupboards with wholegrains such as cereals, oats, brown rice, rye, seeded wholewheat crackers and breads.
- Add oats, nuts or seeds in your cooking, for example, crumbles, toppings.
Fruit and vegetables
Aim to eat 5 portions of fruit or vegetables daily. Fresh, frozen, tinned or dried and juices are all good sources of fibre.
- Eat the washed, edible skins on fresh fruit, such as apples and pears.
- Enjoy fresh, tinned or stewed fruit as a pudding after your main course.
- Add some fresh or dried fruit, nuts or seeds to your breakfast cereal.
- Have some dried fruit, nuts or seeds as a snack between meals.
- Try to have two vegetables with your main meal, for example, carrots and broccoli.
- Add extra vegetables to soups, stews, casseroles and pasta.
- Avoid overcooking vegetables.
- Serve salad vegetables with sandwiches, snacks and packed lunches.
Dietary fibre
Pulses, for example, peas, beans, pearl barley and lentils are an excellent source of fibre. These can add bulk to your stool.
- Have them in stews, soups and casseroles.
- Use baked beans and mushy peas or garden peas with your meals.
Fluids
It is very important to drink plenty of fluids. Have at least eight cups, mugs or glasses daily (1 and half to 2 litres, 3 to 4 pints). Increase the amount of fluid you drink in hot weather and when exercising. A variety of drinks all contribute to your fluid intake.
- Water
- Squashes
- Fruit juices
- Flavoured water
- Milk
- Tea
- Herbal teas
- Coffee
Drinking less than 8 cups could be a cause of constipation. However, over hydrating will not resolve constipation.
Do not ignore the call to have your bowels opened.
Putting off the call to go can be a cause of constipation or lead to urgency. Try to work with the body’s natural rhythm (emptying the bowel first thing in the morning).
Brace and lift technique
The brace and lift technique is used to help coordinate defaecation. We teach this technique with the toilet position. Your nurse will show you how to do brace and lift in clinic and may teach you step by step or ask you to practise daily away from the toilet. Over time you may find you have fewer problems in achieving a complete defecation.
Step 1
- Keeping your shoulders down, take a deep breath that makes your tummy and waist widen like a bellow effect.
- Hold that breath and push out your tummy like a beach ball. You have now created extra abdominal pressure.
- If you now say ‘idge’ you will sense your anus bare down momentarily. This is the first part of the technique helping you to poo.
- Practise the above away from the toilet. How can we use breathing to help with pooing?
Step 2
- To poo, you need the bottom muscles to be relaxed.
- Give your anus muscle a squeeze so that you have lifted that muscle and then relax. Relax again, this is the correct position for pooing.
- From step 1, try saying ‘idge’ at the same time as relaxing your bottom to enable pooing.
You can repeat steps 1 and 2 several times to help pooing.
Bristol stool chart
Type 3 and 4 are classed as normal, easy to pass but also easier to hold on to.
Type 1: Separate hard lumps, like nuts
Type 2: Sausage-like but lumpy
Type 3: Like a sausage but with cracks in the surface
Type 4: Like a sausage or snake, smooth and soft
Type 5: Soft blobs with clear-cut edges
Type 6: Fluffy pieces with ragged edges, a mushy stool
Type 7: Watery, no solid pieces
Toileting position
The best way to sit on the toilet is:
- Legs apart
- Knees higher than hips by either using a foot stool or slowly bring your feet in to tip toe position (avoid doing at speed so as not to contract your pelvic floor)
- Sit upright with your body leaning slightly forward (rest elbows on your thighs).
This position is the best way to assist with complete emptying of the bowel. Privacy and comfort will assist in the complete emptying of your bowels. Try to work with the body’s gastro-colic reflex (body’s natural rhythm), it is at its most powerful first thing in the morning and secondarily post other meals in the day.
Morning routine
- Start the day with a hot drink, like water, lemon, tea or coffee. This helps kick start the body’s rhythm.
- Eat breakfast: This helps to move stools in the bowel, which will in turn help fill the rectum, and increase the urge to have your bowels opened.
- After breakfast, wash and dress or do 10 minutes exercise such as walking or stretches.
- Then sit on the toilet to encourage bowels to empty at a regular time each day (for no longer than ten minutes).
The morning routine can be used with all meals including lunch and dinner.
Remember
When increasing fibre in the diet, introduce the changes gradually, as a sudden increase can cause discomfort and bloating. Aim to increase the number of fibre rich foods you eat gradually over 3 to 5 days. It is important to drink plenty of fluid when increasing your fibre intake. Fibres and fluids work together to ensure a regular, comfortable bowel movement. Try to eat regularly, 3 to 4 meals a day will improve bowel regularity.
Activity
Whatever your activity level, increasing the amount you do will improve your bowel function. Aim for 30 minutes of activity a day, for example, walking, aerobics or chair aerobics, gardening, housework, cycling, swimming or team sports.
If you are unable to achieve this for health or mobility reasons speak to your GP for advice.
Having a urinary catheter is a helpful treatment for many service users but sometimes problems can occur. Proper care of your catheter will reduce the risk of getting problems.
Reducing the risk of urine infections
Having a catheter increases your risk of getting a urine infection as it is easier for bacteria to enter your bladder.
Catheter infections can be serious and difficult to treat.
Sometimes the infections can be life threatening.
Hand washing and keeping clean helps reduce the risk of getting urine infections.
Hand washing
- You should always wash your hands thoroughly with soap and water before and after dealing with your catheter and drainage bags.
- Carers should always wash their hands thoroughly with soap and water before and after dealing with your catheter and drainage bags and should also wear a new pair of disposable gloves each time.
Keeping clean
- Wash the area where the catheter enters your body every day with mild soap and water.
- Wash the area after you have opened your bowels and if the area gets dirty.
- Avoid using talc or creams.
- Have a daily shower or bath if possible.
- Do not remove your leg bag when you have a shower or bath.
- Dry your leg bag by patting it with a clean towel.
Contact your nurse to discuss
Discuss if it is possible to:
- try without your catheter
- use a catheter valve (a discreet product to use instead of a leg
bag) - do intermittent catheterisation (use a removable catheter to periodically drain urine from your bladder, this may have less risk of urine infections)
Contact your nurse
if you would like any advice leaflets:
- sex and catheters
- disposal of continence products
- advice for patients using catheter valves.
Contact your nurse if you would like to discuss any other concerns about your catheter. Your nurse’s telephone number should be at the front of your file or patient notes.
Possible problems
What to do if your catheter is not draining
- Check the tubing is not kinked or squashed.
- If possible try changing your position or walking about.
- Check your drainage bag which may be full and need emptying.
- Check your drainage bag is below the level of your bladder.
- If it is still not draining contact your nurse.
Your catheter is leaking (bypassing) where it enters your body
- Check the tubing is not kinked, pulled or squashed.
- If possible try changing your position or walking about.
- If leaking is an ongoing problem contact your nurse.
Your catheter gets pulled out or falls out
- Contact your nurse.
You may have a urine infection and need to contact your nurse or doctor if you feel unusually unwell and have any of the following:
- A fever
- Pain near your bladder or lower back pain
- Blood in your urine
- Unusual confusion
- Unusual tiredness
- Feeling like you want to vomit or you are vomiting.
Changing your leg bag correctly
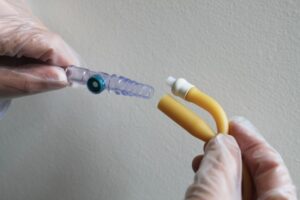
- This will help reduce the risk of urine infections.
- Only change your leg bag every seven days or if it gets dirty or damaged.
- When you change your leg bag, do not touch the tip of the tube (which gets pushed into your catheter).
- Never reuse a leg bag after it has been removed.
Emptying your leg bag
- Do not let your leg bag get too full and heavy as it will pull and damage your body.
- Empty your bag when it is two thirds full.
- Empty your bag into a clean toilet, jug or urinal.
Connecting your night bag correctly
- This will help reduce the risk of urine infections.
- Use a new night bag every night.
- Connect your night bag to your leg bag.
- Do not touch the tip of the night bag tube (which get pushed into your leg bag).
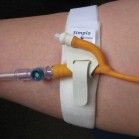
Securing and supporting your catheter and drainage bags
- This helps reduce the risk of pulling and harm to your body and bladder.
- Secure the catheter to your leg or tummy with a securing device (speak to your nurse if you do not have a securing device).
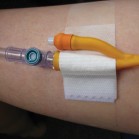
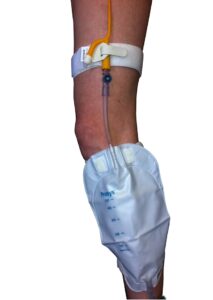
- Support your leg bag by either elastic straps or a stretchy sleeve.

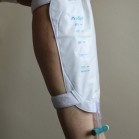

- Support your night bag by a floor stand or bed hanger.
- Never leave your drainage bag touching the floor as it may pick up bacteria.
- Ensure your drainage bags are always positioned below the level of your bladder to help the urine drain.
Fluids
- Drink at least 1 and half to 2 litres (2 and half to 3 and half pints) a day (unless advised otherwise by a healthcare professional).
- This may help reduce the risk of infections.
Bowels
- Eat a healthy diet to avoid constipation as this may cause blocking or leaking of your catheter.
- Speak to your nurse or doctor if you suffer from regular constipation.
Storage of catheters and catheter products
- Store your products in a clean, cool and dry place out of direct sunlight in their original packaging.
- Dispose of products if they are passed their expiry date or if the packaging has been damaged.
Disposal of used catheters and catheter products
- Place used products into two plastic bags before putting them into your household waste bin.
- If you have an infection ask your nurse for advice as you may need to use a special bin.
- This may help to reduce the risk of spreading infection.
References
- Guidelines for urinary catheterisation: adults and children (urethral, supra pubic and intermittent). NHS Leeds Community Healthcare February 2009 Catheter care, RCN guidance for nurses. The Royal College of Nursing March 2008
Patient self-help information
These pages are for patients to find more information about their specific needs.


