
Audiology (ICAN)
We work with children and infants with hearing impairments early in life so that their conditions can be managed as well as possible.
About the audiology (ICAN) service
Operating as part of the integrated children’s additional needs (ICAN) Service we identify children, aged 0 to 18 years who attend a Leeds school or GP, with a hearing impairment early in life so that the condition can be managed as well as possible. We work with the child and family to consider all health and wellbeing issues and then refer to other health services as required.
Referral
Referrals accepted from any healthcare professionals include:
- GPs
- Paediatricians
- School nurses
- Health visitors
- Speech and language therapists
- Community nursery nurse
- School hearing screening programme
- Newborn hearing screening programme
These professionals can refer using the audiology referral form
Read about our referral criteria below.
Patient information
It is important that a hearing loss is identified as soon as possible. A hearing loss can sometimes cause children to have difficulties with communication and socialising. This information tells you about some of the tactics that could help reduce the impact a hearing loss may be having on a child, helping them to feel more understood and less frustrated.
- Before speaking, firstly get your child’s attention by calling their name or by touch. Speak clearly, but don’t shout. If repetition is needed, try using different words.
- Avoid giving instructions or having important discussions in a noisy surrounding. Turning down any music or the television when you are talking to your child may help.
- Try talking face to face, sitting or bending to your child’s face level. It can be helpful to have light on your face and avoid standing in front of a window which can make lip reading difficult.
- When talking with your child, check that they are listening and watching. Check as you go along that they have understood. It is important to be aware, that when tired, listening can be harder work for your child.
- Don’t forget to inform relatives and friends who have contact with your child of the hearing difficulties your child may be experiencing. When informing your child’s teacher, ask if they can move your child to the front of the class. The teacher will also be able to let you know if your child needs any extra help at home or school.
Community audiology is a team of professionals who specialise in testing children’s hearing. This information tells you about some of the hearing tests we use. We hope this will help you talk to your child about what will happen when they come to clinic.
The distraction test
- If your baby can sit unsupported, distraction testing can be used.
- Your baby will sit on your knee with you holding them around the waist.
- One tester will keep your baby’s attention by playing with some toys.
- The other tester will make a range of different sounds from behind your baby.
- We want to see if your baby will turn to look when they hear the sound.
- The sounds will be low, middle and high pitched.
- The sounds will start off quiet and get louder.
- We want to find the quietest sound at each pitch that your baby will turn for.
- It is very important that you don’t give any clues when the sound is there.

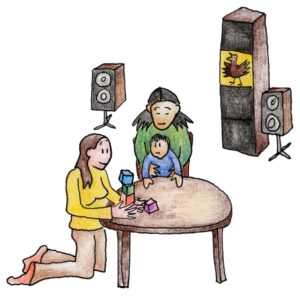
Visual reinforcement audiometry
- Visual reinforcement audiometry can be used to test babies who can sit unsupported, and toddlers.
- Your child will sit on your knee with you holding them around the waist.
- On each side of the room are two speakers, with cabinets with toys that light up inside.
- One tester will keep your child’s attention by allowing them to play with some toys on the table.
- The other tester will work the test equipment.
- Your child will be shown that when a sound comes, a toy lights up.
- This will encourage your child to turn around each time they hear the sound.
- We want to find the quietest sound at each pitch that your child will turn for.
- It is very important that you don’t give any clues when the sound is there.
Performance test
- Older toddlers and pre school children may be able to do a performance test.
- One tester will stand behind your child with an electronic “Warbler” which makes sounds of known pitch and volume.
- The other tester will show your child the “game”: when they hear the sound they put a man in the boat.
- When your child plays the game they will be tested with low, medium and high pitched sounds. The sounds will start off loud and get quieter.
- The gaps between the sounds are changed to make sure they are not guessing.
- We want to find the quietest sound that your child can hear at each pitch.

Pure tone audiometry
- Pure tone audiometry is used with older pre-school children and school age children.
- The child listens for different tones through headphones.
- Each time they hear a tone they put a peg in a pegboard: older children and teenagers are given a button to press.
- The tones start off loud and get quieter until they are no longer heard.
- Pure tone audiometry tells us the quietest sound that can be heard in each ear, at each pitch tested.

The toy test
- The toy test is used with older toddlers and pre-school children.
- The tester puts some toys out on the table in front of your child.
- The toys are in pairs and are chosen because they sound similar, for example, key and tree.
- Your child will be asked to point to a toy.
- The tester will make sure your child can’t lip-read.
- The tester’s voice level is measured.
- This test is used to see how well your child can hear speech.

| Name of clinic or clinical pathway | Children’s community audiology services |
|---|---|
| Narrative description of the clinic or clinical pathway | The service identifies children, aged 0 to 18 years, who attend a Leeds school or GP, with a hearing impairment early in life so that the condition can be best managed. |
| Who can refer? | Referrals accepted from any healthcare professionals include:
|
| Who can’t refer? |
|
| What intervention is expected by the referrer before a referral is made? |
|
Referral Criteria:
|
|
Inclusions |
Exclusions (including referral route) |
|
|
Newborn hearing screener (Newborn Hearing Screening Programme)
Newborn hearing screening helps identify babies who have permanent hearing loss as early as possible. These babies and their families can then get the support and advice they need right from the start.
A newborn hearing screener will offer to test your baby’s hearing, usually before you are discharged. Otherwise you can attend an out-patient appointment within the first few weeks.
If the screening results do not show a clear response from one or both of your baby’s ears, an appointment will be made with the hospital audiologist for further testing.
Community audiologist (children’s community audiology Service)
A community audiologist tests children’s hearing, aged 0-18 years, in health centres across the city. They can identify children with hearing loss and discuss suitable management options depending on the degree of loss and current difficulties the child may be experiencing. Children with health conditions associated with possible hearing loss are also monitored in our clinics.
Community paediatrician (Aetiological Medicine)
A community paediatrician is a doctor specialising in children’s health with an interest in hearing problems. They are trained to find out the causes and diagnose the type of hearing loss or balance disorder your child has. They can also offer advice on and assist in the treatment and management of the hearing loss.
Teacher of the Deaf (Deaf and Hearing Impairment team (DAHIT))
An educational audiologist and teacher of the Deaf works with children and families in their homes, early years settings, local schools, or further education settings. They provide advice and training to ensure that families and staff in settings have the knowledge and skills to support the development and achievement of their child or young person.
Hospital audiologist (hearing and balance services)
The audiologists at Seacroft hospital tests children’s hearing aged 0 to 25 and then offer a seamless transition to the adult service. Babies and children can be referred here for more specialised hearing tests and to confirm any deafness. If hearing aids are offered as a management option, these will be fitted to your child’s individual needs and their progress with the hearing aids will be monitored in close collaboration with the teacher of the Deaf.
Speech and language therapist (DAHIT Speech and Language Therapy Clinic)
A specialist speech and language therapist (SLT) works with babies and children with a diagnosed hearing loss in Leeds. You may see a SLT in a variety of settings including at home, in school or nursery. A SLT will offer support for families, school and nursery staff to develop the communication skills of deaf and hearing impaired babies and children.
Ear, nose and throat consultant (Ear, nose and throat services)
An ear, nose, and throat specialist looks after hearing problems. Your ENT doctor’s role is to identify any causes of hearing loss and if there are any medical or surgical treatments that may help. A treatment can range from something relatively simple, like removing wax, treating infection or placing grommets to more complex surgeries. The ENT doctor may also recommend your child has imaging studies (CT or MRI scans) to further understand the type and source of hearing loss. The doctor may also need to check your child’s ears are suitable for hearing aid fitting. If it is felt that your child may benefit from a cochlear implant, the ENT doctor, along with the audiologist will refer you onto a specialist centre for additional assessments and counselling prior to surgery.
How we work together
Collectively we are a group of professionals who are passionate about providing the best care to deaf children and their families in Leeds.
The team fosters a joint, positive approach to deafness and aims to provide a seamless journey as our families move throughout the different services, as shown below.
We recognise the need for individuality of each child and their family and value parents as equal members of the team.


